Warts: Types, Causes, Symptoms & Risk Factors — The Complete Guide
You notice a rough, raised bump on your hand. Or a small, flat patch on your child’s face. Or a painful, hard lump on the bottom of your foot that makes walking uncomfortable. Before you reach for a home remedy or ignore it entirely, it is worth understanding exactly what warts on skin are, why they appear, and what they mean for your health.
Warts on skin are among the most common viral skin infections in the world, yet they remain widely misunderstood. Many people do not realise that all types of warts are caused by the same virus — the Human Papillomavirus (HPV) — or that different strains of HPV produce dramatically different warts with distinct appearances, locations, and treatment needs.
This guide covers everything you need to know about warts on skin: all the types of warts and how to recognise each one, the biological causes and transmission routes, the full symptom picture, the risk factors that make some people more susceptible than others, and when warts on skin require professional warts removal treatment rather than watchful waiting.
What Are Warts on Skin?
Warts on skin are small, non-cancerous growths caused by an infection with the Human Papillomavirus (HPV). There are more than 200 strains of HPV, and different strains infect different areas of the body — producing the distinct types of warts that dermatologists classify and treat differently.
The HPV virus infects the outermost layer of the skin (the keratinocytes of the epidermis) through tiny cuts, abrasions, or compromised areas of the skin barrier. Once inside, the virus causes the infected skin cells to multiply abnormally rapidly — producing the characteristic raised, rough, or thickened growth we recognise as warts on skin. The virus does not infect deeper tissues, which is why warts on skin are benign. They are confined to the surface layers.
Warts are not dangerous in the conventional sense — they do not become cancerous in most cases and often resolve on their own as the immune system clears the HPV infection. However, they are contagious, they can spread to other areas of the same person’s body, they can be painful in specific locations, and some types of warts on skin — particularly genital warts — are associated with strains of HPV that carry a higher clinical risk and require prompt attention from a dermatologist.
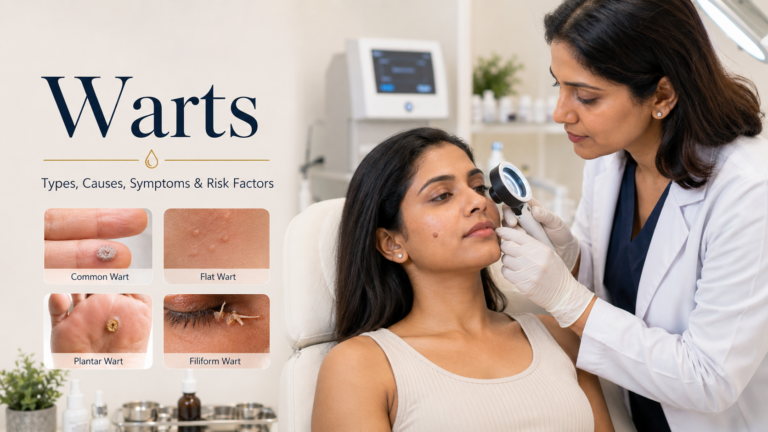
Types of Warts on Skin — How to Identify Each One
Understanding the types of warts on skin matters because each type looks different, appears in different locations, and responds differently to warts removal treatment. Here is a complete breakdown of all types of warts and how to recognise them.
- Common Warts on Hands (Verruca Vulgaris)
Common warts on hands are the most frequently encountered of all types of warts on skin. Caused by HPV strains 2 and 4, they appear most often on the fingers, knuckles, and backs of hands — though they can occur anywhere on the body. The texture is unmistakable: rough, raised, and dome-shaped, with a surface that resembles a tiny cauliflower. Look closely and you may see tiny black dots within the wart — these are clotted blood vessels, not seeds, and their presence is a reliable sign that you are looking at common warts on hands or fingers.
Warts on fingers treatment is among the most common warts removal requests at dermatology clinics because common warts on hands spread easily through direct contact and through touching shared surfaces. Children are particularly susceptible to common warts on hands due to frequent skin-to-skin contact and the minor cuts and abrasions that come with physical play.
- Plantar Warts on Feet (Verruca Plantaris)
Plantar warts on feet are a distinct type of warts on skin that develop on the soles, heels, and balls of the feet — areas that bear the body’s weight. Unlike other types of warts, plantar warts on feet grow inward rather than outward, driven into the skin by the pressure of standing and walking. This is why plantar warts often feel like a hard, painful pebble under the foot rather than a visible raised bump.
Plantar warts on feet are easily recognised by a thickened, callous-like patch of skin with a small, dark centre — again, those telltale clotted blood vessels. They frequently occur in clusters (a configuration called mosaic warts) and are caused by HPV strains 1, 2, and 4. Plantar warts on feet are contracted through direct contact with contaminated surfaces — swimming pools, gym changing rooms, and communal showers are all common transmission sites. The warm, moist environments of these spaces make plantar wart infection significantly more likely.
Plantar warts on feet can be stubbornly resistant to warts treatment at home and typically require professional warts removal treatment for complete resolution, particularly when they occur in clusters or when the pain is affecting daily movement.
- Flat Warts on Face and Skin (Verruca Plana)
Flat warts on face, legs, and arms are smaller and smoother than other types of warts on skin — their flattened, slightly raised surface makes them easy to mistake for other skin conditions at first glance. They tend to be skin-coloured, pink, or lightly pigmented, and they appear in large numbers: it is common to find dozens of flat warts clustered together in the same area.
Flat warts on face are caused by HPV strains 3 and 10 and spread rapidly through shaving — which is why they appear along shaving paths in men and across the legs in women who shave. Children frequently develop flat warts on the face and forehead. Because flat warts on face are subtle in appearance, many patients dismiss them as post-acne marks or uneven skin tone for months before seeking evaluation from a dermatologist.
- Filiform Warts (Thread Warts)
Filiform warts are thin, thread-like projections of warts on skin that grow rapidly and typically appear on the face — specifically around the eyes, nose, mouth, and neck. They are longer and more finger-like than other types of warts, and though they look alarming, they are among the easiest warts to treat when addressed early. Filiform warts are caused by HPV strains 1, 2, and 4 and can be spread by touching or scratching the affected area.
- Periungual Warts (Around and Under the Nails)
Periungual warts develop around and beneath the fingernails and toenails, creating rough, uneven clusters of warts on skin that can distort the nail plate, interfere with nail growth, and become painful. They are particularly common in people who bite their nails or pick at their cuticles, as these habits create the micro-abrasions through which HPV enters the skin. Warts on fingers treatment under the nail is one of the more challenging warts removal procedures because the anatomy limits access — and leaving periungual warts untreated risks permanent nail damage.
- Genital Warts — The Most Clinically Important Type
Genital warts are caused by HPV strains 6 and 11 — strains classified as low-risk for cancer but high-priority for medical attention because of their transmission route (sexual contact) and their association with other HPV strains that do carry cancer risk. Genital warts appear as soft, flesh-coloured growths in and around the genitals, anus, and inner thighs. They may be single or clustered, flat or raised.
Genital warts treatment is not optional in the way that, say, common warts on hands might be. Genital warts caused by HPV 6 and 11 warrant prompt evaluation by a dermatologist or gynaecologist because: they can be transmitted to sexual partners, they can be confused with other STIs requiring different treatment, they may indicate concurrent infection with higher-risk HPV strains, and they require clinical genital warts treatment — prescription topical agents, cryotherapy, or laser — rather than any form of warts treatment at home.
Warts Causes and Symptoms — What Is Actually Happening in Your Skin
Warts Caused by HPV — The Root Cause
All warts on skin share a single underlying cause: infection with a strain of the Human Papillomavirus. HPV is one of the most widespread viruses in the world — it is estimated that 80% of the global population will be infected with at least one strain of HPV at some point in their lives, according to the World Health Organization (2024).
Warts caused by HPV spread through two primary routes. Direct skin-to-skin contact with an existing wart is the most common transmission pathway — shaking hands with someone who has common warts on hands, for example, can transfer the virus if there is any break in your own skin barrier. The second route is contact with HPV-contaminated surfaces: gym equipment, pool surrounds, shared towels, and bathroom floors all harbour the virus and serve as transmission points, particularly for plantar warts on feet.
The virus enters through cuts, abrasions, eczema patches, bitten nails, or any other compromise in the skin’s protective barrier. Once inside the keratinocytes, it hijacks the cell’s replication machinery to produce new viral particles and stimulate the abnormal cell growth that forms warts on skin. The incubation period — from HPV exposure to visible wart development — ranges from one to eight months, which is why people often cannot identify where or when they contracted the virus.
Symptoms of Warts on Skin — What You Will Notice
The symptoms of warts on skin vary by type, but several features help identify them across the board. Most warts on skin are painless — the exception being plantar warts on feet, which can cause significant discomfort with standing and walking, and periungual warts, which may cause throbbing around the nail bed.
Common symptoms associated with warts on skin include a rough, raised, or hardened bump that differs in texture from the surrounding skin; a skin-coloured, white, pink, or brown growth; tiny black dots within the growth (clotted capillaries); and itching or tenderness around the wart. Flat warts on face and body tend to be smooth rather than rough but still maintain the slightly elevated, discreet appearance that separates them from completely flat skin changes like pigmentation marks.
Warts on skin can change over time. New warts may appear around the original one as the virus spreads through autoinoculation — scratching or picking at warts on skin deposits the virus onto adjacent skin, seeding new warts in the process. This is one of the most important reasons to avoid picking at warts and to seek warts removal treatment early rather than waiting for the warts to multiply.
Warts Risk Factors — Who Is Most Likely to Get Warts on Skin
While anyone can develop warts on skin after HPV exposure, several warts risk factors significantly increase the likelihood of infection, the rate of spread, and the difficulty of achieving successful warts removal treatment.
Age — Children and Young Adults Are Most Vulnerable
Warts on skin are significantly more common in children and young adults — not because HPV exposure is higher in this age group, but because acquired immunity to HPV builds over time. Children who have never been exposed to a particular HPV strain have no existing immune memory to contain it quickly. This is why common warts on hands are so prevalent in school-age children and why outbreaks of flat warts on face are common in school environments. Adults who contracted HPV in childhood often develop immunity that prevents recurrence — but new HPV strains can still cause warts even in adults with prior infection history.
Compromised Immune System — A Major Warts Risk Factor
An impaired immune system is one of the most significant individual warts risk factors. Patients living with HIV, those receiving immunosuppressive therapy after organ transplantation, people undergoing chemotherapy, and patients on long-term corticosteroids all have reduced capacity to suppress HPV replication — meaning warts on skin are more likely to develop, grow faster, resist standard warts removal treatment, and recur after treatment. For immunocompromised patients, warts removal near me is not just a cosmetic concern but a medical priority requiring specialist dermatologist management.
Skin Breaks and Barrier Damage
HPV cannot penetrate intact, healthy skin. Every cut, blister, eczema patch, nail bite wound, or area of dry cracked skin is a potential entry point for the virus. This is why nail biters are disproportionately affected by periungual warts and warts on fingers — the constant micro-trauma creates continuous opportunities for HPV entry. Patients with atopic dermatitis (eczema) are similarly more susceptible to warts on skin because their compromised skin barrier allows HPV access more readily.
Communal Environments — Swimming Pools and Gyms
Shared, warm, moist environments are ideal conditions for HPV survival on surfaces. Swimming pool surrounds, communal changing rooms, gym floors, and shared shower facilities are consistently identified as transmission sites for plantar warts on feet in particular. Walking barefoot in these environments while having any break in the skin of the feet — even a small one — represents meaningful plantar warts risk. Wearing flip-flops in communal areas is a simple, effective prevention strategy.
Frequent Skin-to-Skin Contact with Infected Individuals
Occupations and activities involving frequent hand contact with multiple people — healthcare workers, teachers, childcare providers, physiotherapists, and martial arts practitioners — carry elevated warts risk factors simply due to the volume of skin-to-skin interactions. Household transmission is also common: living with a family member who has warts on skin increases your own warts risk, particularly for children sharing baths and towels.
When to See a Dermatologist for Warts on Skin
Many warts on skin — particularly common warts on hands in children — can be safely monitored without treatment if they are not painful, not spreading, and not causing distress. However, certain situations make professional warts removal treatment necessary rather than optional.
See a dermatologist for warts removal treatment if: your warts on skin are multiplying or spreading to new areas; plantar warts on feet are causing pain that affects your daily movement; warts appear on your face, genitals, or near the eyes; you have tried warts treatment at home for more than three months without improvement; you have any doubt about whether the growth is a wart or something else; or you are immunocompromised, since warts in this setting require specialist management.
Never attempt to cut, burn, or remove warts at home using sharp objects. This spreads the HPV virus, creates wounds that can become infected, and frequently makes subsequent warts removal treatment more difficult. Legitimate warts treatment at home is limited to salicylic acid formulations applied carefully to the surface of non-facial, non-genital warts — and even these should be discussed with a dermatologist first for guidance on correct use.
Warts Removal Treatment Options — What Clinical Options Are Available
Effective warts removal treatment exists across a range of modalities, and the best approach depends on the type of warts, their location, the patient’s age and immune status, and how long the warts on skin have been present. At Vesta Skin, Dr. Uma evaluates all of these factors before recommending a warts removal treatment protocol.
Cryotherapy remains the most widely used first-line warts removal treatment for common warts on hands, plantar warts on feet, and flat warts on face. Liquid nitrogen is applied to the wart, freezing and destroying the infected tissue. Multiple cryotherapy sessions spaced two to three weeks apart are typically required for complete warts removal treatment — the number depends on the size and depth of the wart.
Salicylic acid is the mainstay of warts treatment at home for simple common warts on hands and plantar warts on feet. Prescription-strength formulations (17–40%) are more effective than over-the-counter versions and work by chemically exfoliating the surface layers of the wart over several weeks. Warts treatment at home with salicylic acid is most effective on small, early warts and should be used consistently — daily application after soaking the skin — for a minimum of eight to twelve weeks.
Laser treatment for warts on skin uses pulsed dye laser or CO2 laser to destroy the blood vessels feeding the wart or to ablate the wart tissue directly. Laser warts removal treatment is particularly effective for plantar warts on feet that have not responded to cryotherapy, for periungual warts, and for warts in locations where cryotherapy carries a risk of scarring. It is the most effective single modality for stubborn, recurrent warts on skin — and the most precise.
Immunotherapy involves stimulating the body’s own immune response to fight the HPV infection directly. Intralesional injections of antigens such as Candida or MMR antigen trigger a localised immune reaction that spreads systemically, clearing not just the injected wart but often multiple warts simultaneously. This makes immunotherapy particularly valuable for patients with extensive or recurrent warts on skin who have not responded to standard warts removal treatment.
Genital warts treatment requires prescription topical agents — imiquimod or podophyllotoxin — applied at home under a dermatologist’s guidance, or clinic-based procedures including cryotherapy, laser, or surgical excision depending on the extent and distribution of the genital warts. Over-the-counter warts treatment at home products should never be used on genital warts.
Frequently Asked Questions — Warts on Skin
- Are warts on skin contagious?
Yes — warts on skin are highly contagious. They spread through direct contact with an existing wart, through shared surfaces contaminated with HPV, and through autoinoculation (touching your own wart and then touching another area of skin). Common warts on hands are particularly easy to transmit through handshakes and shared objects. Plantar warts on feet spread readily in communal pool and gym environments. This is one of the strongest reasons to seek warts removal treatment early rather than waiting.
- What causes warts on skin to appear?
All warts on skin are caused by strains of the Human Papillomavirus (HPV). The virus enters through breaks or abrasions in the skin and triggers abnormal multiplication of surface skin cells — producing the characteristic growth. Warts caused by HPV are more likely to develop in people with compromised skin barriers (cuts, eczema, nail biting), weakened immune systems, and those who frequently contact HPV-contaminated surfaces like gym floors and swimming pools.
- Can warts on skin go away on their own?
Yes — approximately 65% of warts on skin in people with healthy immune systems resolve spontaneously within two years as the body’s immune system clears the HPV infection. However, warts removal treatment significantly reduces this timeline by an average of 70% and eliminates the risk of the warts spreading further during the waiting period. Plantar warts on feet, periungual warts, and genital warts rarely resolve quickly on their own and typically warrant warts removal treatment.
- What is the difference between plantar warts on feet and a corn?
Plantar warts on feet and corns can look similar — both cause thickened, hardened skin on the sole — but they are fundamentally different. Plantar warts on feet contain tiny black dots (clotted blood vessels) within the thickened skin and may be painful when squeezed from the sides rather than from direct pressure. Corns are caused by friction and pressure, not HPV, have no black dots, and are most painful with direct pressure. A dermatologist can definitively distinguish between plantar warts on feet and corns with a clinical examination.
- Is warts treatment at home effective?
Warts treatment at home with salicylic acid is effective for simple common warts on hands and plantar warts on feet, particularly when the warts are small and have been present for less than a year. It requires consistent daily application for eight to twelve weeks and works by slowly exfoliating the wart tissue. Warts treatment at home should never be used on facial warts, genital warts, or warts on irritated skin. For warts that are large, painful, spreading, or have not responded to three months of warts treatment at home, professional warts removal near me is the appropriate next step.
- Where can I get warts removal treatment near me in Chennai?
Vesta Skin by Dr. Uma offers comprehensive warts assessment and warts removal treatment in T Nagar, Chennai. Dr. Uma evaluates the type, location, and duration of your warts on skin before recommending the most appropriate warts removal treatment — from cryotherapy and salicylic acid protocols to laser warts removal for stubborn or recurrent cases. Book your free consultation at vestaskin for wart treatment in Chennai with a qualified dermatologist.
Conclusion — What You Need to Know About Warts on Skin
Warts on skin are among the most common dermatological conditions in the world — caused by HPV, transmitted through skin contact and shared surfaces, and manifesting in distinct types across different body areas. Understanding the types of warts, recognising the causes and symptoms, and knowing the warts risk factors that increase your susceptibility gives you the information you need to make sensible decisions about whether to monitor warts on skin or seek professional warts removal treatment.
The key points to remember: all types of warts are caused by strains of HPV; most warts on skin in healthy individuals eventually resolve without treatment, but warts removal treatment dramatically accelerates that process and prevents transmission; warts treatment at home is appropriate only for simple, non-genital, non-facial warts; and any warts on skin that are spreading, painful, on the face or genitals, or not responding to home care after three months warrant assessment by a qualified dermatologist.
Key takeaways:
- All warts on skin are caused by HPV — different strains cause different types of warts in different locations
- Common warts on hands and plantar warts on feet are the most prevalent — spread through contact and shared surfaces
- Flat warts on face spread easily through shaving; filiform and periungual warts require early treatment to prevent complications
- Genital warts treatment is not optional — seek clinical assessment promptly
- Warts risk factors include young age, weakened immunity, broken skin, and communal wet environments
- Warts removal treatment options include cryotherapy, salicylic acid, laser, and immunotherapy — the best choice depends on the type and location